The statistics about pelvic pain are startling. 1 in 4 women and 1 in 11 men will experience pelvic pain in their lifetime.
Navigating pelvic pain can be like navigating the labyrinth—there can be a lot of twists and turns on your way to your center of relief. In addition to traditional medical interventions like injections, medications, physical therapy, what can you do to help yourself feel better?
Here are eight strategies you may find helpful to relieve pelvic pain.
1. Use your breath

The breath and nervous system
Conscious breathwork, or pranayama, has been shown to decrease heart rate and decrease blood pressure.
Because pain is an output of the nervous system, retraining the brain is crucial. The use of pranayama, or breath work, is particularly helpful for this reason. Working with your breath asks the nervous system to shift the balance of fight or flight (sympathetic nervous system) to rest and digest (parasympathetic nervous system).
We can think of the two arms of the autonomic nervous system as the gas and the break. If we are in a lot of pain, our sympathetic nervous system, as the gas, adds more cortisol into our bloodstream.
When we apply the break, or parasympathetic nervous system, we decrease the stress response. This is one reason why pranayama is beneficial for people experiencing persistent pain.
The mechanics of breathing
Another reason why breathing is helpful for people experiencing pelvic pain is the relationship between the diaphragm and the pelvic floor.
When you inhale, both your diaphragm and pelvic floor descend toward your feet. When you exhale, they ascend toward your head. This helps provide a piston-like motion to the system. Each breath cycle offers range of motion of your pelvic floor and support to your low back and pelvis.
Often when you’re stressed, there’s a tendency to breathe more shallow. Shallow breaths means your belly doesn’t expand as much and the ribs don’t glide outwards away from the midline of your body during inhalation. This means you won’t get the full benefit of the diaphragm and pelvic floor descending and ascending.
Read more about different types of pranayama, like Dirgha and Nadi Shodhana.
2. Nourish your nervous system

While we are on the topic of the nervous system, you can be creative with finding ways to nourish it, like with sipping warm tea, using aromatherapy, or other ideas you’ll discover in this blog on 10 ways to nourish your nervous system. Support your parasympathetic nervous system so it can help you decrease and manage pain.
3. Pay attention to your posture
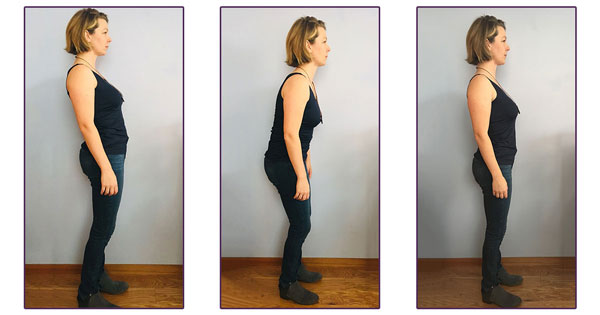
What is an ideal sitting posture? As I mentioned in my recent blog about sitting posture, slumped sitting can affect the function of the pelvic floor muscles. While I argue there may not be such a thing as “bad sitting posture,” you may find relief in stacking your pelvis and spine in a neutral position.
If sitting bothers you, standing may be a good alternative. I have a makeshift standing workstation that I find helpful to relieve pressure on my back and coccyx, but it is also important to be mindful of how you stand.
If you trade slumped sitting for slumped standing, is standing actually any better? Read more about how standing posture affects your back and pelvic health.
4. Roll out your feet


Did you know the connective tissue on the bottom of your feet is continuous all the way up to the pelvis?
Here is a fun trick for you to try. Pretest with a forward bend, as if you were about to touch your toes, and notice which muscle groups feel tight.
Come back in standing, place a pinky ball on the ground, and roll out your arch from your heel to the ball of your foot. Roll back and forth for a minute and switch to the other side. (Note: you can also use a tennis ball or a lacrosse ball, but I find the pinky ball is less slippery than a tennis ball and softer than a lacrosse ball.)
Retest your forward bend. Did anything change? Were you able to descend further and/or with more ease?
5. You are what you eat

The old adage is true. I have witnessed many patients report less pain and better bowel health when they adjust what food they put into their body.
Some patients notice they have less pain when eliminating dietary triggers. This may include caffeine, bladder irritants, dairy, gluten, or sugar. People who have been diagnosed with interstitial cystitis are familiar with how food and beverages can increase pain and urinary frequency/urgency. Bladder pain is not the only diagnosis that nutrition can influence. Check out my colleague Jessica Drummond’s work on holistic nutrition for people with pelvic pain.
6. Bowel health

Bowel health is important for a few reasons. Many people feel better if they have regular bowel movements, which helps avoid bloating and abdominal pain. Regular bowel movements can also decrease urinary leakage and pelvic pain.
My pediatric pelvic health teacher and nationally recognized physical therapist, Dawn Sandalcidi, taught me a big lesson in her pediatric course about the importance of bowel movements. She told us that we must help clear constipation first for kiddos who are experiencing bedwetting or urinary leakage during the day. When stool gets backed up in the sigmoid colon, it creates less space for the bladder and can contribute to leakage.
The same thing goes for adults. When there is stool backed up in the rectum people are more likely to experience urinary leakage.
We also see a high incidence of constipation in people experiencing pelvic pain. This is sometimes caused by tightness of one of the inner muscles of the pelvic floor, puborectalis, pulling the rectum forward and not allowing an easy passage of stool. Elongation and relaxation of the pelvic floor muscles helps manage constipation of a mechanical nature.
For people experiencing coccyx or vaginal pain, the extra pressure on the pelvic floor muscles can sometimes make the pain worse.
If this is a concern for you, there are ways you can optimize your bowel health.
7. Yoga

Yes, of course yoga makes my list!
As discussed above, when you decrease the overactivity of the sympathetic nervous system, you calm the fight/flight/freeze response. Yoga is one way to do this.
- Yoga increases the pliability of muscles and connective tissue, increasing flexibility in the myofascial attachments to the pelvis and trunk. This allows the nerves to have the space they need to slide, glide, and not get irritated.
- Yoga helps people discover a pain-free range of motion by increasing body awareness. It is crucial for us to reprogram the brain to change the imprint that movement is expected to be dangerous or painful.
- Yoga helps integrate the mind, body and spirit. People who experience chronic pain often disassociate from the body part that is disrupting their life. A yoga practice helps renew the relationship with the physical body.
8. Meditation

Meditation has been shown to decrease depression symptoms and increase quality of life for people with chronic pelvic pain.
The evidence compiled from 30 randomized controlled trials* is not strong enough to say that pain is statistically significantly lowered.
So why did meditation make the list for my favorite strategies to reduce pelvic pain if there isn’t statistically strong evidence behind it? Any tool that is non-invasive and offers support in coping wins in my book! Also, mindfulness practices (different than meditation) are also very helpful in combating day to day stress, anxiety and pain.
I hope you found this overview helpful! I look forward to reading your comments below about what strategies work for you!
*Hilton, L., Hempel, S., Ewing, B. A., Apaydin, E., Xenakis, L., Newberry, S., Colaiaco, B., Maher, A. R., Shanman, R. M., Sorbero, M. E., Maglione, M. A. (2016). Mindfulness Meditation for Chronic Pain: Systematic Review and Meta-analysis. Annals of behavioral medicine : a publication of the Society of Behavioral Medicine, 51(2), 199-213.







Love this!!!!!
So glad it was helpful! Thanks for letting me know!
Thank you for taking the time to create this list. It will be my Go To list for 2019. Your words empower and educate.
Thanks so much for the feedback. I think it can be helpful to have a list of strategies to try when the going gets rough. I hope you feel better ASAP!
Thank you so much for sharing with us. This is what I was searching for. It’s so valuable for me, and I love this article, primarily how you have explained everything in detail.
I’m so happy to hear that Jenny! Thanks for sharing!